2026-04-24
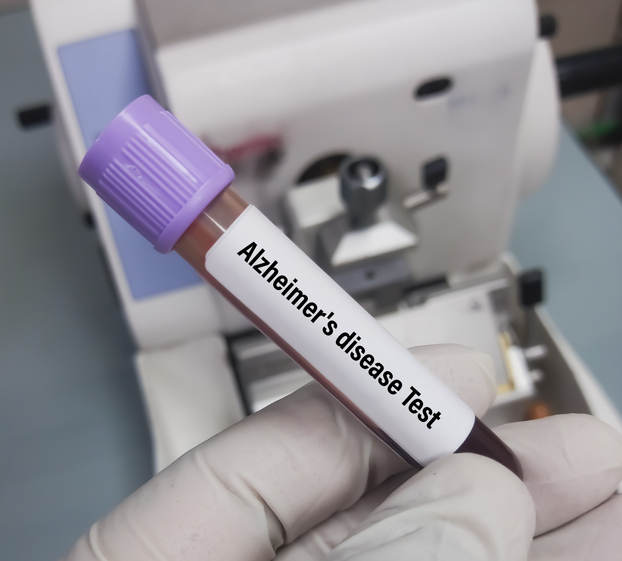
Alzheimer’s disease: tau protein spreads along neural networks
Neurology
By Elodie Vaz | Published on April 24,
2026 | 3 min read
Alzheimer’s disease, the most common form of dementia, is characterized by progressive neurodegeneration. It initially affects memory, then gradually impairs all cognitive functions, ultimately compromising daily independence. Biologically, two major lesions are involved: extracellular deposits of beta-amyloid peptides and intracellular aggregates of tau protein.
Normally involved in stabilizing neuronal microtubules, tau becomes pathological when it aggregates into neurofibrillary tangles, contributing to neuronal death and cognitive decline.
A study published on April 8, 2026, in Neuron addresses a key question that remains poorly understood: the mechanism by which tau pathology spreads through the brain. Although the progressive distribution of lesions follows a well-described pattern—from the temporal lobe to the neocortex—the exact mechanisms of this propagation remain hypothetical. The researchers therefore aimed to determine whether and how tau aggregates move between neurons and across brain networks.
To reach their conclusions, the researchers analyzed post-mortem brain samples and longitudinal data from 128 participants in the ROSMAP cohort, followed for nearly ten years. Two brain regions were examined for each individual: the inferior temporal lobe, involved in episodic memory, and the superior frontal lobe, associated with executive functions.
The approach integrates multiple levels of analysis: quantification of tau “seeds,” individual genetic data, and functional magnetic resonance imaging (fMRI) acquired prior to death. The use of Mendelian randomization allowed the team to infer causal relationships between the presence of these seeds and the formation of neurofibrillary tangles.
As explained in a press release by Jeremy Herskowitz, MD, PhD, professor of neurology and neurobiology at UAB and lead author of the study: “We used a genetic approach called Mendelian causality to conclude that neuronal seeds generated in the temporal cortex were responsible for neurofibrillary tangle pathology in the neocortex.”
The findings provide converging evidence supporting trans-synaptic propagation of tau protein. “Small fragments of tau protein aggregate within neurons and spread from neuron to neuron throughout the brain,” he adds. “Neurons are interconnected and communicate via synapses, allowing these aggregates to travel through the brain […] until they reach the neocortex.”
The study shows that this spread preferentially follows each individual’s neural networks. In other words, brain connectivity determines the trajectory, distance, and potentially the speed of propagation of tau aggregates. Interindividual differences in neural “wiring” thus directly influence the extent of tau pathology.
This work represents “the most extensive investigation to date of the bioactivity of tau protein aggregates in the human brain,” combining, for the first time, post-mortem data with fMRI. The results confirm that tau seeds originating in the temporal cortex play a causal role in spreading pathology to broader cortical regions.
These findings strengthen the hypothesis of active propagation of tau pathology along neural circuits, providing a mechanistic basis for the anatomical progression of Alzheimer’s disease. “This is a major advance […] both for the development of therapies and for understanding how the disease works,” the researcher emphasizes.
From a therapeutic perspective, the results shed light on the potential mechanism of action of anti-tau antibodies. “Anti-tau antibodies could prevent tau protein from spreading from one brain region to another. If this propagation can be stopped, it may delay or even prevent Alzheimer’s disease.”
Precisely identifying these propagation pathways opens the door to strategies targeting not only tau protein itself but also the neural networks involved. Future research will need to clarify the cellular and synaptic mechanisms at play in order to translate this understanding into clinical interventions capable of modifying the natural course of the disease.
Read next: Alzheimer’s disease: a direct link with fine particulate matter
About the Author – Elodie Vaz
Health journalist, CFPJ graduate (2023).
Élodie explores the marks diseases leave on bodies and, more broadly, on human life. A registered nurse since 2010, she spent twelve years at patients’ bedsides before exchanging her stethoscope for a notebook. She now investigates the links between environment and health, convinced that the vitality of life cannot be reduced to that of humans alone.
Alzheimer’s disease, the most common form of dementia, is characterized by progressive neurodegeneration. It initially affects memory, then gradually impairs all cognitive functions, ultimately compromising daily independence. Biologically, two major lesions are involved: extracellular deposits of beta-amyloid peptides and intracellular aggregates of tau protein.
Normally involved in stabilizing neuronal microtubules, tau becomes pathological when it aggregates into neurofibrillary tangles, contributing to neuronal death and cognitive decline.
A study published on April 8, 2026, in Neuron addresses a key question that remains poorly understood: the mechanism by which tau pathology spreads through the brain. Although the progressive distribution of lesions follows a well-described pattern—from the temporal lobe to the neocortex—the exact mechanisms of this propagation remain hypothetical. The researchers therefore aimed to determine whether and how tau aggregates move between neurons and across brain networks.
Combining brain connectivity and molecular biology
To reach their conclusions, the researchers analyzed post-mortem brain samples and longitudinal data from 128 participants in the ROSMAP cohort, followed for nearly ten years. Two brain regions were examined for each individual: the inferior temporal lobe, involved in episodic memory, and the superior frontal lobe, associated with executive functions.
The approach integrates multiple levels of analysis: quantification of tau “seeds,” individual genetic data, and functional magnetic resonance imaging (fMRI) acquired prior to death. The use of Mendelian randomization allowed the team to infer causal relationships between the presence of these seeds and the formation of neurofibrillary tangles.
Brain connectivity: a key driver of tau spread
As explained in a press release by Jeremy Herskowitz, MD, PhD, professor of neurology and neurobiology at UAB and lead author of the study: “We used a genetic approach called Mendelian causality to conclude that neuronal seeds generated in the temporal cortex were responsible for neurofibrillary tangle pathology in the neocortex.”
The findings provide converging evidence supporting trans-synaptic propagation of tau protein. “Small fragments of tau protein aggregate within neurons and spread from neuron to neuron throughout the brain,” he adds. “Neurons are interconnected and communicate via synapses, allowing these aggregates to travel through the brain […] until they reach the neocortex.”
The study shows that this spread preferentially follows each individual’s neural networks. In other words, brain connectivity determines the trajectory, distance, and potentially the speed of propagation of tau aggregates. Interindividual differences in neural “wiring” thus directly influence the extent of tau pathology.
Targeting tau propagation: a promising therapeutic strategy
This work represents “the most extensive investigation to date of the bioactivity of tau protein aggregates in the human brain,” combining, for the first time, post-mortem data with fMRI. The results confirm that tau seeds originating in the temporal cortex play a causal role in spreading pathology to broader cortical regions.
These findings strengthen the hypothesis of active propagation of tau pathology along neural circuits, providing a mechanistic basis for the anatomical progression of Alzheimer’s disease. “This is a major advance […] both for the development of therapies and for understanding how the disease works,” the researcher emphasizes.
From a therapeutic perspective, the results shed light on the potential mechanism of action of anti-tau antibodies. “Anti-tau antibodies could prevent tau protein from spreading from one brain region to another. If this propagation can be stopped, it may delay or even prevent Alzheimer’s disease.”
Precisely identifying these propagation pathways opens the door to strategies targeting not only tau protein itself but also the neural networks involved. Future research will need to clarify the cellular and synaptic mechanisms at play in order to translate this understanding into clinical interventions capable of modifying the natural course of the disease.
Read next: Alzheimer’s disease: a direct link with fine particulate matter
About the Author – Elodie Vaz
Health journalist, CFPJ graduate (2023).
Élodie explores the marks diseases leave on bodies and, more broadly, on human life. A registered nurse since 2010, she spent twelve years at patients’ bedsides before exchanging her stethoscope for a notebook. She now investigates the links between environment and health, convinced that the vitality of life cannot be reduced to that of humans alone.
Last press reviews
Malaria Vaccine: Finally a Turning Point ?
By Ana Espino | Published on April 23, 2026 | 4 min read<br><br><br>...
Alzheimer’s disease: tau protein spreads along neural networks

By Elodie Vaz | Published on April 24, 2026 | 3 min read<br>
Childhood dementia: synaptic hyperactivity as an early trigger in a brain in decline

By Elodie Vaz | Published on Avril 23, 2026 | 3 min read<br><br><br>