2026-05-20
Diabetes: the gut, a new target of metformin
Endocrinology and Metabolism
By Elodie Vaz | Published on May 20,
2026 | 4 min read
For decades, metformin has been regarded as a drug that acts primarily on the liver to reduce glucose production. But a new study conducted by Northwestern University and published on May 8 in Nature Metabolism challenges this paradigm: the true site of its action may actually be the intestine. In mice, researchers show that the drug works by directly modifying the energy metabolism of intestinal cells, effectively turning the intestine into a “glucose sponge.”
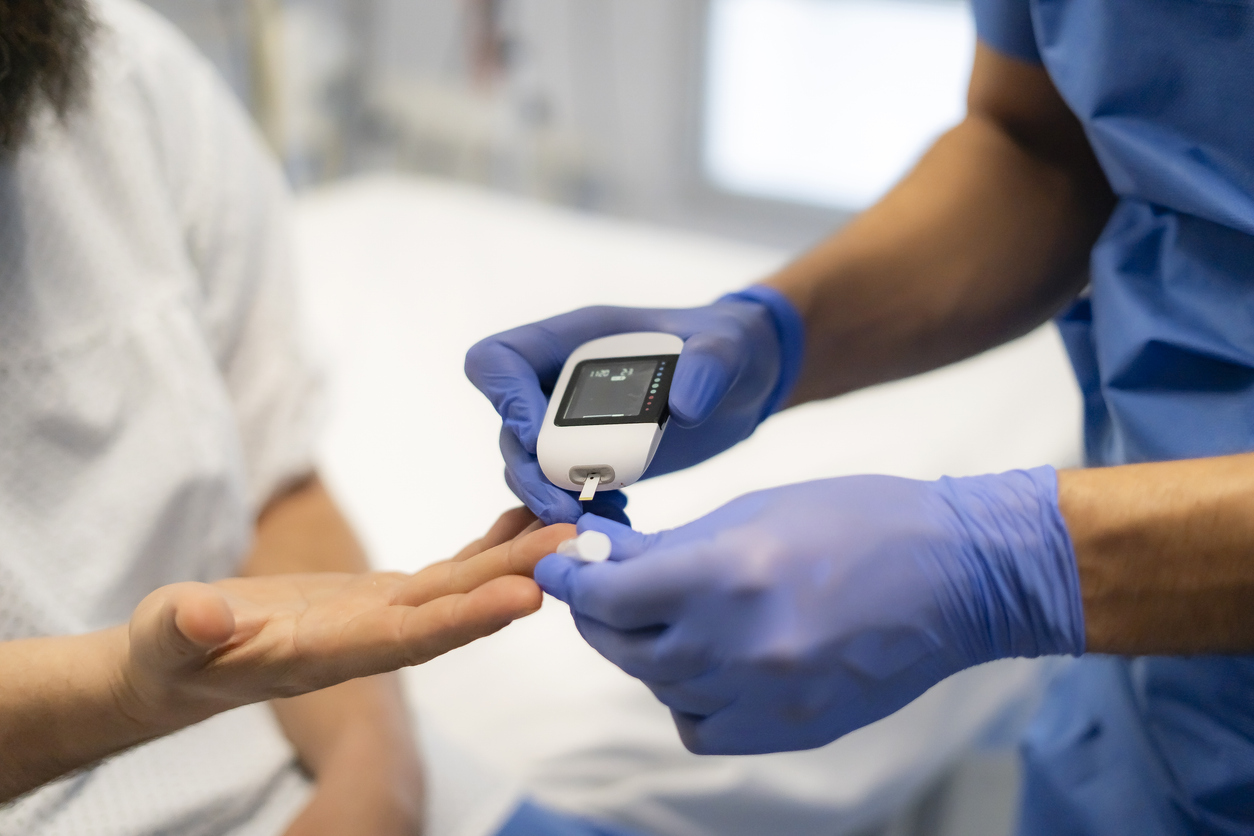
Type 2 diabetes is characterized by chronic hyperglycemia linked to progressive insulin resistance. When the body can no longer properly use glucose, it accumulates in the bloodstream, increasing the risk of vascular, renal, neurological, and cardiovascular complications. For several decades, metformin has been the first-line treatment used to control excessive blood sugar levels.
Until now, the scientific consensus held that the molecule mainly reduced hepatic glucose production. However, several clinical observations remained difficult to explain, including its pronounced effect after meals, its ability to reduce appetite, and its multiple metabolic effects.
The aim of this new study was precisely to identify the tissue truly responsible for metformin’s therapeutic effects. The work builds on previous research from Navdeep Chandel’s laboratory, which had already shown that the drug inhibits mitochondrial complex I, an enzyme essential for cellular respiration and energy production.
The key question, however, remained unanswered: in which organ does this inhibition produce the metabolic effects observed in patients? “Metformin essentially helps the intestine absorb glucose from the blood, which further highlights the intestine’s major role in blood sugar regulation,” explained Dr. Navdeep Chandel, senior author of the study and professor of biochemistry and molecular genetics at the Feinberg School of Medicine, in a press release.
To answer this question, the researchers used a mouse model expressing a yeast enzyme, NDI1, capable of mimicking mitochondrial complex I while remaining resistant to inhibition by metformin.
This enzyme was expressed specifically in the intestinal cells of the mice, rendering only the intestine insensitive to the drug. The researchers then observed the effects on blood glucose levels in treated animals.
The results showed that when intestinal mitochondria could no longer be inhibited by metformin, the drug’s glucose-lowering effect was significantly reduced. These findings demonstrate that the intestine may be a major — if not central — site of the molecule’s therapeutic action.
Intestinal
mitochondria at the heart of blood sugar control
The study shows that metformin slows mitochondrial energy production in intestinal mucosal cells. This energy deficit then forces the cells to consume more glucose in order to maintain their metabolic activity.
In other words, the intestine actively captures circulating sugar, thereby reducing blood glucose levels after meals. This discovery also helps explain several phenomena long observed in patients taking metformin.
Researchers notably reported reduced circulating levels of citrulline, a molecule produced exclusively by the mitochondria of the small intestine, as well as increased levels of GDF15, a hormone associated with reduced appetite and weight loss. “We’ve always wondered how one drug could have ten different effects,” said Dr. Chandel. “Well, it’s possible if it targets a key component of the cell, and targeting mitochondria is a key component.”
The study also highlights unexpected similarities with berberine, a dietary supplement widely promoted on social media. According to the authors, berberine appears to use the same intestinal metabolic pathway as metformin.
The researchers nevertheless urge caution. “Metformin is supported by decades of clinical evidence, whereas supplements like berberine are far less studied,” Dr. Chandel emphasized.
Beyond metformin itself, this study opens the door to a new therapeutic approach centered on the intestine and intestinal mitochondria. According to Professor Zach Sebo, these findings invite researchers to reassess established models: “Our study suggests that revisiting assumptions about metformin’s mechanism of action could lead to a better understanding of how it works.”
About the Author – Elodie Vaz
Health journalist, CFPJ graduate (2023).
Élodie explores the marks diseases leave on bodies and, more broadly, on human life. A registered nurse since 2010, she spent twelve years at patients’ bedsides before exchanging her stethoscope for a notebook. She now investigates the links between environment and health, convinced that the vitality of life cannot be reduced to that of humans.
For decades, metformin has been regarded as a drug that acts primarily on the liver to reduce glucose production. But a new study conducted by Northwestern University and published on May 8 in Nature Metabolism challenges this paradigm: the true site of its action may actually be the intestine. In mice, researchers show that the drug works by directly modifying the energy metabolism of intestinal cells, effectively turning the intestine into a “glucose sponge.”
Type 2 diabetes is characterized by chronic hyperglycemia linked to progressive insulin resistance. When the body can no longer properly use glucose, it accumulates in the bloodstream, increasing the risk of vascular, renal, neurological, and cardiovascular complications. For several decades, metformin has been the first-line treatment used to control excessive blood sugar levels.
Until now, the scientific consensus held that the molecule mainly reduced hepatic glucose production. However, several clinical observations remained difficult to explain, including its pronounced effect after meals, its ability to reduce appetite, and its multiple metabolic effects.
Rethinking metformin’s mechanism of action
The aim of this new study was precisely to identify the tissue truly responsible for metformin’s therapeutic effects. The work builds on previous research from Navdeep Chandel’s laboratory, which had already shown that the drug inhibits mitochondrial complex I, an enzyme essential for cellular respiration and energy production.
The key question, however, remained unanswered: in which organ does this inhibition produce the metabolic effects observed in patients? “Metformin essentially helps the intestine absorb glucose from the blood, which further highlights the intestine’s major role in blood sugar regulation,” explained Dr. Navdeep Chandel, senior author of the study and professor of biochemistry and molecular genetics at the Feinberg School of Medicine, in a press release.
To answer this question, the researchers used a mouse model expressing a yeast enzyme, NDI1, capable of mimicking mitochondrial complex I while remaining resistant to inhibition by metformin.
This enzyme was expressed specifically in the intestinal cells of the mice, rendering only the intestine insensitive to the drug. The researchers then observed the effects on blood glucose levels in treated animals.
The results showed that when intestinal mitochondria could no longer be inhibited by metformin, the drug’s glucose-lowering effect was significantly reduced. These findings demonstrate that the intestine may be a major — if not central — site of the molecule’s therapeutic action.
Intestinal
mitochondria at the heart of blood sugar control
The study shows that metformin slows mitochondrial energy production in intestinal mucosal cells. This energy deficit then forces the cells to consume more glucose in order to maintain their metabolic activity.
In other words, the intestine actively captures circulating sugar, thereby reducing blood glucose levels after meals. This discovery also helps explain several phenomena long observed in patients taking metformin.
Researchers notably reported reduced circulating levels of citrulline, a molecule produced exclusively by the mitochondria of the small intestine, as well as increased levels of GDF15, a hormone associated with reduced appetite and weight loss. “We’ve always wondered how one drug could have ten different effects,” said Dr. Chandel. “Well, it’s possible if it targets a key component of the cell, and targeting mitochondria is a key component.”
The study also highlights unexpected similarities with berberine, a dietary supplement widely promoted on social media. According to the authors, berberine appears to use the same intestinal metabolic pathway as metformin.
The researchers nevertheless urge caution. “Metformin is supported by decades of clinical evidence, whereas supplements like berberine are far less studied,” Dr. Chandel emphasized.
A new therapeutic target?
Beyond metformin itself, this study opens the door to a new therapeutic approach centered on the intestine and intestinal mitochondria. According to Professor Zach Sebo, these findings invite researchers to reassess established models: “Our study suggests that revisiting assumptions about metformin’s mechanism of action could lead to a better understanding of how it works.”
Read next: Liver, sugar, and pills: who's in control?
About the Author – Elodie Vaz
Health journalist, CFPJ graduate (2023).
Élodie explores the marks diseases leave on bodies and, more broadly, on human life. A registered nurse since 2010, she spent twelve years at patients’ bedsides before exchanging her stethoscope for a notebook. She now investigates the links between environment and health, convinced that the vitality of life cannot be reduced to that of humans.
Last press reviews
Remdesivir: a real turning point against COVID-19?

By Ana Espino | Published on May 12, 2026 | 4 min read<br><br><br>C...
Frequent placental contractions at the heart of normal pregnancies

By Elodie Vaz | Published on May 12, 2026 | 4 min read<br><br><br>...
Hantavirus: how does the virus hijack the cell?
By Ana Espino | Published on May 11, 2026 | 4 min read<br><br><br><br>