2026-04-17
Hemophilia: a revolution in a single injection?
Hematology
By Ana Espino | Published on April 17, 2026 | 4 min read
Hemophilia is a rare genetic disorder characterized by a deficiency in coagulation factor VIII (hemophilia A) or IX (hemophilia B). This condition leads to recurrent bleeding episodes that can result in severe complications such as joint damage, chronic pain, and, in some cases, life-threatening hemorrhages. Beyond its clinical impact, hemophilia significantly affects the quality of life of patients and their families.
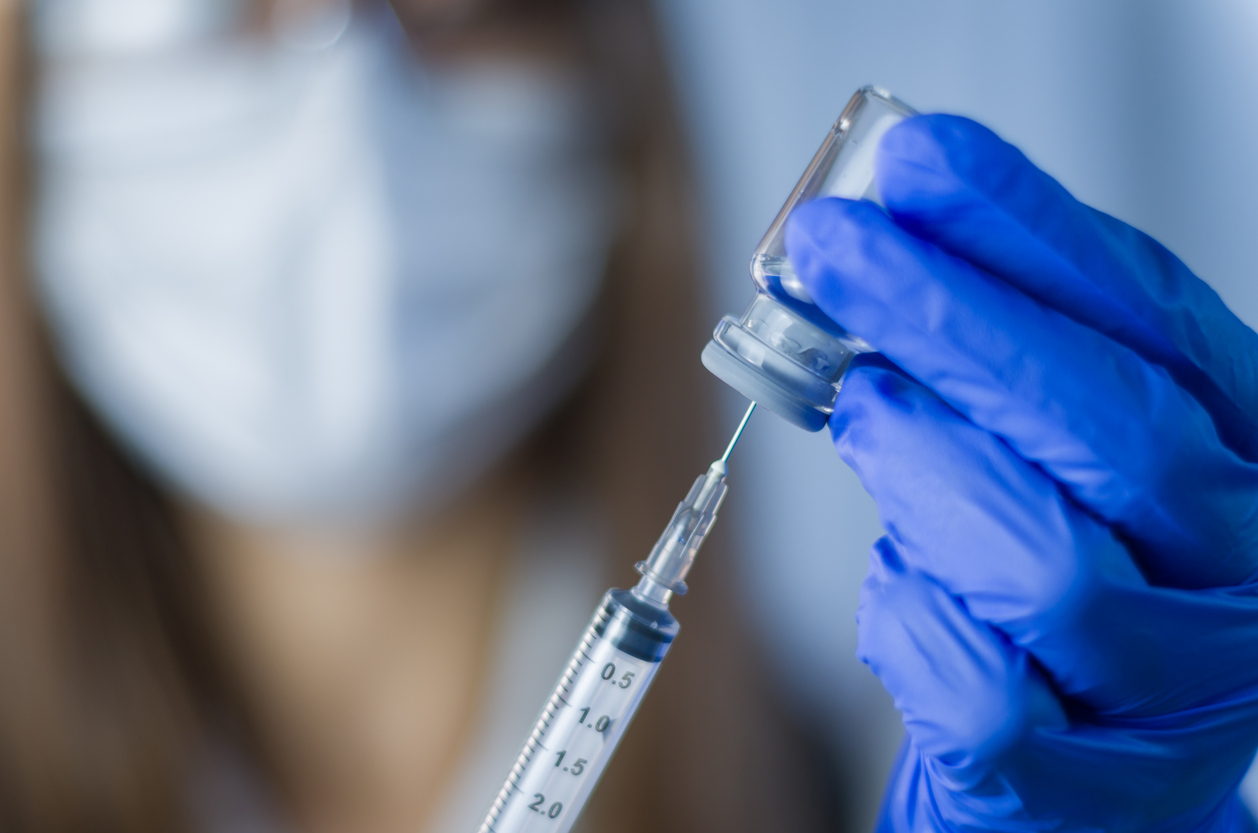
Despite therapeutic advances, current treatments have major limitations. Replacement therapies require lifelong regular injections, which are often burdensome and costly. In addition, the development of neutralizing antibodies against administered factors reduces their effectiveness. Non-replacement therapies, although innovative, do not completely eliminate the risk of bleeding, particularly in cases of trauma.
In this context, several challenges remain: improving treatment durability, reducing therapeutic burden, limiting immune responses, and expanding access to patients, particularly pediatric populations.
Against this backdrop, gene therapy appears to be a promising strategy. The aim of this review is to analyze the main approaches under development—AAV vectors, lentiviral vectors, and genome editing—in order to assess their potential, limitations, and future perspectives.
This study is based on a comprehensive review of available preclinical and clinical data on the different gene therapy strategies for hemophilia. It examines mechanisms of action, clinical trial outcomes, as well as the advantages and limitations of each approach.
AAV-based gene therapies are currently the most advanced clinically. They have demonstrated a significant increase in coagulation factor levels, accompanied by a marked reduction in bleeding episodes and reliance on conventional treatments. However, these approaches are limited by immune responses, particularly hepatic ones, sometimes requiring prolonged immunosuppression. In addition, their efficacy may be compromised in patients with pre-existing antibodies, and durability remains variable, especially in hemophilia A.
Lentiviral approaches offer a major advantage: integration of the therapeutic gene into the genome, allowing potentially long-term expression, including in dividing cells. This opens interesting prospects, particularly for pediatric patients. However, these strategies are still at an early stage and carry risks, notably related to conditioning regimens and insertional mutagenesis, which may lead to serious adverse effects.
Finally, genome editing techniques such as CRISPR-Cas9 represent an innovative approach aimed at directly correcting the genetic defect underlying the disease. They offer curative potential with high precision. Nevertheless, these technologies are still in early development and raise concerns regarding off-target effects and delivery challenges.
Overall, these approaches show encouraging results, with improved disease control, but still require optimization to ensure long-term safety and efficacy.
Hemophilia, as a chronic genetic disease, remains associated with a significant therapeutic burden and substantial complications. Current challenges mainly concern treatment durability, management of immune responses, and access to these new therapies for all patients, especially children.
This study aimed to evaluate advances in different gene therapy approaches, highlighting their benefits and limitations. The results confirm that gene therapy represents a major breakthrough, with the potential to transform hemophilia management by offering single-administration treatments with long-lasting—or even curative—effects.
However, some limitations persist, including limited long-term data, uncertainties regarding the durability of coagulation factor expression, and constraints related to patient eligibility. Nevertheless, the outlook is promising. Future research should improve the safety and efficacy of these approaches, overcome immunological barriers, and extend these innovations to broader patient populations. Genome editing, in particular, could ultimately provide a durable curative solution for all patients with hemophilia.
About the author – Ana Espino
PhD in Immunology, specialized in Virology
As a scientific writer, Ana is passionate about bridging the gap between research and real-world impact. With expertise in immunology, virology, oncology, and clinical studies, she makes complex science clear and accessible. Her mission: to accelerate knowledge sharing and empower evidence-based decisions through impactful communication.
Hemophilia is a rare genetic disorder characterized by a deficiency in coagulation factor VIII (hemophilia A) or IX (hemophilia B). This condition leads to recurrent bleeding episodes that can result in severe complications such as joint damage, chronic pain, and, in some cases, life-threatening hemorrhages. Beyond its clinical impact, hemophilia significantly affects the quality of life of patients and their families.
Despite therapeutic advances, current treatments have major limitations. Replacement therapies require lifelong regular injections, which are often burdensome and costly. In addition, the development of neutralizing antibodies against administered factors reduces their effectiveness. Non-replacement therapies, although innovative, do not completely eliminate the risk of bleeding, particularly in cases of trauma.
In this context, several challenges remain: improving treatment durability, reducing therapeutic burden, limiting immune responses, and expanding access to patients, particularly pediatric populations.
Against this backdrop, gene therapy appears to be a promising strategy. The aim of this review is to analyze the main approaches under development—AAV vectors, lentiviral vectors, and genome editing—in order to assess their potential, limitations, and future perspectives.
Does gene therapy really work ?
This study is based on a comprehensive review of available preclinical and clinical data on the different gene therapy strategies for hemophilia. It examines mechanisms of action, clinical trial outcomes, as well as the advantages and limitations of each approach.
AAV-based gene therapies are currently the most advanced clinically. They have demonstrated a significant increase in coagulation factor levels, accompanied by a marked reduction in bleeding episodes and reliance on conventional treatments. However, these approaches are limited by immune responses, particularly hepatic ones, sometimes requiring prolonged immunosuppression. In addition, their efficacy may be compromised in patients with pre-existing antibodies, and durability remains variable, especially in hemophilia A.
Lentiviral approaches offer a major advantage: integration of the therapeutic gene into the genome, allowing potentially long-term expression, including in dividing cells. This opens interesting prospects, particularly for pediatric patients. However, these strategies are still at an early stage and carry risks, notably related to conditioning regimens and insertional mutagenesis, which may lead to serious adverse effects.
Finally, genome editing techniques such as CRISPR-Cas9 represent an innovative approach aimed at directly correcting the genetic defect underlying the disease. They offer curative potential with high precision. Nevertheless, these technologies are still in early development and raise concerns regarding off-target effects and delivery challenges.
Overall, these approaches show encouraging results, with improved disease control, but still require optimization to ensure long-term safety and efficacy.
How far can these new approaches go ?
Hemophilia, as a chronic genetic disease, remains associated with a significant therapeutic burden and substantial complications. Current challenges mainly concern treatment durability, management of immune responses, and access to these new therapies for all patients, especially children.
This study aimed to evaluate advances in different gene therapy approaches, highlighting their benefits and limitations. The results confirm that gene therapy represents a major breakthrough, with the potential to transform hemophilia management by offering single-administration treatments with long-lasting—or even curative—effects.
However, some limitations persist, including limited long-term data, uncertainties regarding the durability of coagulation factor expression, and constraints related to patient eligibility. Nevertheless, the outlook is promising. Future research should improve the safety and efficacy of these approaches, overcome immunological barriers, and extend these innovations to broader patient populations. Genome editing, in particular, could ultimately provide a durable curative solution for all patients with hemophilia.
Read next: Fitusiran: what if we rebalanced coagulation?
About the author – Ana Espino
PhD in Immunology, specialized in Virology
As a scientific writer, Ana is passionate about bridging the gap between research and real-world impact. With expertise in immunology, virology, oncology, and clinical studies, she makes complex science clear and accessible. Her mission: to accelerate knowledge sharing and empower evidence-based decisions through impactful communication.
Last press reviews
What If Nanotechnology Redefined the Future of Sunscreens?

By Ana Espino | Published on June 05, 2026 | 4 min read<br>
Cervical Cancer: Could the Microbiome Play a Key Role Alongside HPV?

By Ana Espino | Published on June 03, 2026 | 4 min read<br>
Hantavirus: Why Does This Rare Virus Continue to Concern Intensive Care Specialists?
By Ana Espino | Published on June 03, 2026 | 4 min read<br>