2026-03-04
Less blood, less fear: a revolution in pediatric dentistry
Dentistry
By Ana Espino | Published on March 4, 2026 | 3 min read
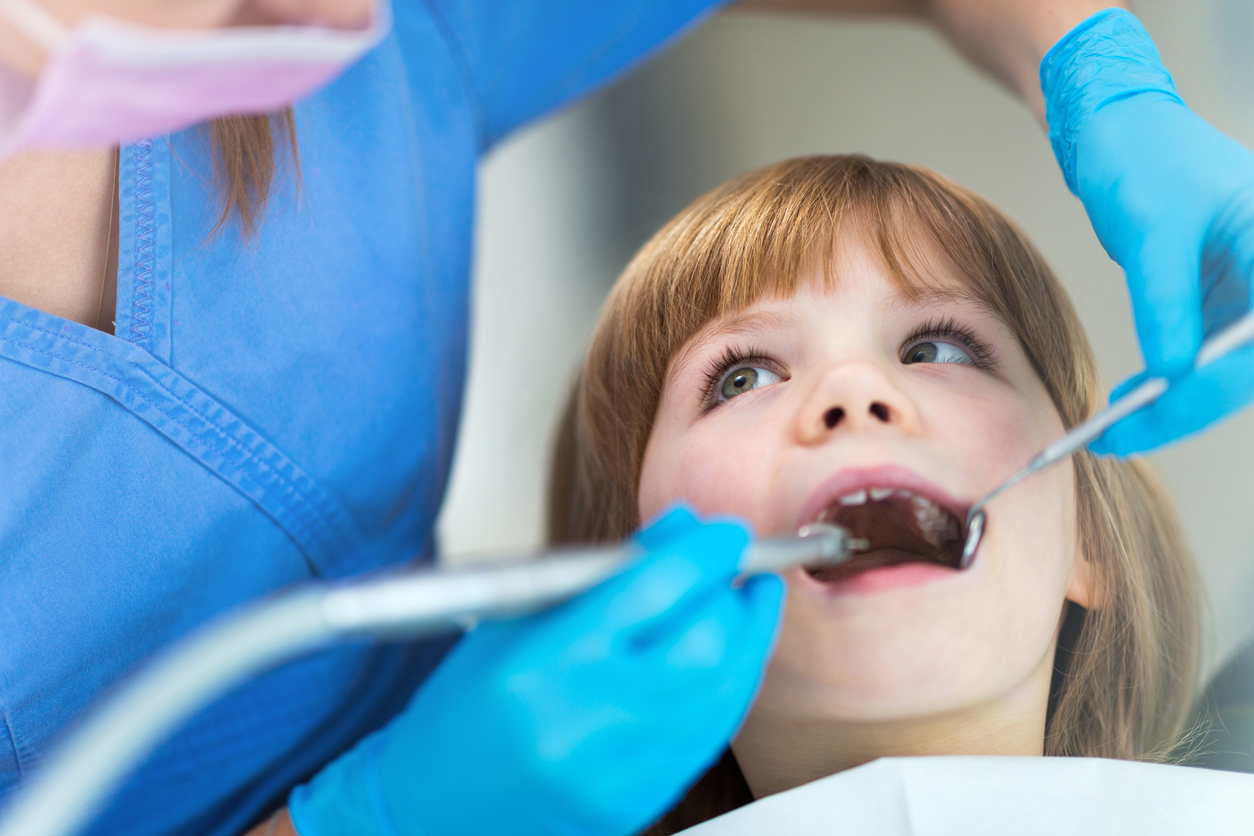
Fear of blood and pain represents a major barrier to dental care in children. This often underexpressed preoperative anxiety negatively affects therapeutic adherence and has a lasting impact on the perception of future care. In pediatric oral surgery, many procedures—extractions, biopsies, or excision of benign lesions—are associated with visible bleeding, which can heighten apprehension and negatively influence the operative experience.
The conventional scalpel, historically regarded as the reference tool because of its precision and ease of use, nevertheless presents limitations in pediatric practice. Intraoperative bleeding can reduce visibility of the surgical field, prolong procedure time, and increase postoperative edema or discomfort. These technical and psychological constraints have encouraged the development of so-called “bloodless” techniques aimed at optimizing hemostasis while minimizing tissue trauma.
The review published in 2025 in the Journal of Pharmacy and Bioallied Sciences analyzes the mechanisms of action, clinical indications, as well as the benefits and limitations of the main approaches used to achieve a bloodless operative field in pediatric dentistry: electrosurgery, laser therapy, cryosurgery, and Apexum.
The authors present a narrative review of contemporary techniques that create a bloodless operative field in pediatric dentistry. The objective is to assess their mechanisms of action, clinical indications, and benefit–risk profiles.
Electrosurgery, introduced in the early twentieth century, relies on the application of high-frequency electrical current that enables simultaneous cutting and coagulation of soft tissues. It is indicated for gingivectomy, frenectomy, exposure of impacted teeth, and biopsy procedures. It provides effective hemostasis, reduces operative time, and limits postoperative discomfort. However, it is contraindicated in patients with pacemakers and in certain procedures close to bone tissue.
Lasers, introduced into dentistry in the 1960s, produce a photothermal reaction that induces protein coagulation above 60°C and tissue ablation above 100°C. They are used for benign mucosal lesions, gingival hyperplasia, mucoceles, and aesthetic procedures. Their precision reduces peripheral necrosis, improves operative visibility, and decreases postoperative pain. Nevertheless, caution is required in cardiac and immunocompromised patients.
Cryosurgery, based on the cytotoxic effect of extreme cold, allows controlled destruction of benign lesions such as fibromas, leukoplakia, or lichen planus. It is associated with a low rate of secondary infection, minimal scarring risk, and generally does not require local anesthesia. However, certain systemic conditions constitute formal contraindications.
Finally, the Apexum technique represents a minimally invasive approach in endodontics. It enables removal of inflamed periapical tissues through the root canal, without surgical flap elevation or suturing. This method promotes faster healing and reduces postoperative pain while preserving the benefits of traditional apical surgery.
Pediatric oral surgery faces a dual imperative: ensuring therapeutic efficacy while preserving the child’s emotional balance. Control of intraoperative bleeding is not merely a technical issue but also a major lever for reducing anxiety and improving treatment acceptance.
This review aimed to evaluate contemporary approaches designed to limit or eliminate bleeding in pediatric practice. The analyzed data indicate that electrosurgery, lasers, cryosurgery, and the Apexum technique improve operative field visibility, ensure effective hemostasis, and reduce tissue trauma. These benefits translate into decreased postoperative discomfort and an improved overall clinical experience.
Although their use requires careful case selection and appropriate technical expertise, these technologies illustrate the shift toward less invasive and better-tolerated pediatric surgery. In the long term, their rational integration may enhance treatment adherence, improve procedural safety, and sustainably optimize clinical outcomes in pediatric dentistry.
About the author – Ana Espino
PhD in Immunology, specialized in Virology
As a scientific writer, Ana is passionate about bridging the gap between research and real-world impact. With expertise in immunology, virology, oncology, and clinical studies, she makes complex science clear and accessible. Her mission: to accelerate knowledge sharing and empower evidence-based decisions through impactful communication.
Fear of blood and pain represents a major barrier to dental care in children. This often underexpressed preoperative anxiety negatively affects therapeutic adherence and has a lasting impact on the perception of future care. In pediatric oral surgery, many procedures—extractions, biopsies, or excision of benign lesions—are associated with visible bleeding, which can heighten apprehension and negatively influence the operative experience.
The conventional scalpel, historically regarded as the reference tool because of its precision and ease of use, nevertheless presents limitations in pediatric practice. Intraoperative bleeding can reduce visibility of the surgical field, prolong procedure time, and increase postoperative edema or discomfort. These technical and psychological constraints have encouraged the development of so-called “bloodless” techniques aimed at optimizing hemostasis while minimizing tissue trauma.
The review published in 2025 in the Journal of Pharmacy and Bioallied Sciences analyzes the mechanisms of action, clinical indications, as well as the benefits and limitations of the main approaches used to achieve a bloodless operative field in pediatric dentistry: electrosurgery, laser therapy, cryosurgery, and Apexum.
What if surgery became invisible to the child?
The authors present a narrative review of contemporary techniques that create a bloodless operative field in pediatric dentistry. The objective is to assess their mechanisms of action, clinical indications, and benefit–risk profiles.
Electrosurgery, introduced in the early twentieth century, relies on the application of high-frequency electrical current that enables simultaneous cutting and coagulation of soft tissues. It is indicated for gingivectomy, frenectomy, exposure of impacted teeth, and biopsy procedures. It provides effective hemostasis, reduces operative time, and limits postoperative discomfort. However, it is contraindicated in patients with pacemakers and in certain procedures close to bone tissue.
Lasers, introduced into dentistry in the 1960s, produce a photothermal reaction that induces protein coagulation above 60°C and tissue ablation above 100°C. They are used for benign mucosal lesions, gingival hyperplasia, mucoceles, and aesthetic procedures. Their precision reduces peripheral necrosis, improves operative visibility, and decreases postoperative pain. Nevertheless, caution is required in cardiac and immunocompromised patients.
Cryosurgery, based on the cytotoxic effect of extreme cold, allows controlled destruction of benign lesions such as fibromas, leukoplakia, or lichen planus. It is associated with a low rate of secondary infection, minimal scarring risk, and generally does not require local anesthesia. However, certain systemic conditions constitute formal contraindications.
Finally, the Apexum technique represents a minimally invasive approach in endodontics. It enables removal of inflamed periapical tissues through the root canal, without surgical flap elevation or suturing. This method promotes faster healing and reduces postoperative pain while preserving the benefits of traditional apical surgery.
A paradigm shift in pediatric dentistry
Pediatric oral surgery faces a dual imperative: ensuring therapeutic efficacy while preserving the child’s emotional balance. Control of intraoperative bleeding is not merely a technical issue but also a major lever for reducing anxiety and improving treatment acceptance.
This review aimed to evaluate contemporary approaches designed to limit or eliminate bleeding in pediatric practice. The analyzed data indicate that electrosurgery, lasers, cryosurgery, and the Apexum technique improve operative field visibility, ensure effective hemostasis, and reduce tissue trauma. These benefits translate into decreased postoperative discomfort and an improved overall clinical experience.
Although their use requires careful case selection and appropriate technical expertise, these technologies illustrate the shift toward less invasive and better-tolerated pediatric surgery. In the long term, their rational integration may enhance treatment adherence, improve procedural safety, and sustainably optimize clinical outcomes in pediatric dentistry.
Read next: AI in dentistry
About the author – Ana Espino
PhD in Immunology, specialized in Virology
As a scientific writer, Ana is passionate about bridging the gap between research and real-world impact. With expertise in immunology, virology, oncology, and clinical studies, she makes complex science clear and accessible. Her mission: to accelerate knowledge sharing and empower evidence-based decisions through impactful communication.
Last press reviews
Malaria Vaccine: Finally a Turning Point ?
By Ana Espino | Published on April 23, 2026 | 4 min read<br><br><br>...
Alzheimer’s disease: tau protein spreads along neural networks
By Elodie Vaz | Published on April 24, 2026 | 3 min read<br>
Childhood dementia: synaptic hyperactivity as an early trigger in a brain in decline

By Elodie Vaz | Published on Avril 23, 2026 | 3 min read<br><br><br>